Diabetes: Misunderstood, yet so many around us live with it
Diabetes has affected thousands of Americans alone
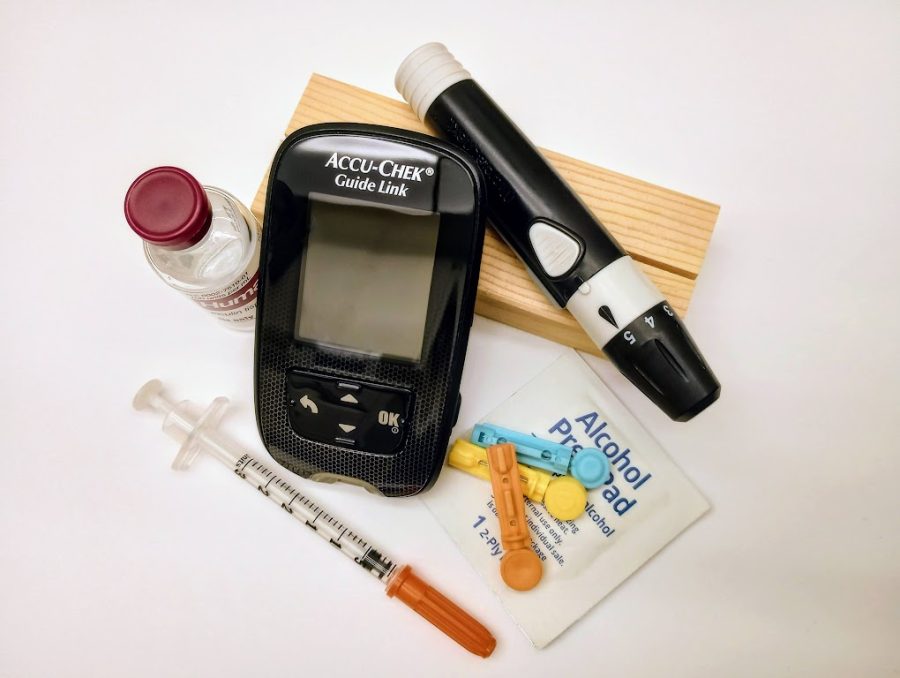
A photo of some equipment used to manage diabetes and check blood sugar levels. A small bottle of insulin, a syringe, a glucometer, small needles for blood samples, alcohol wipes, and a pen needle.
LOS ALAMITOS, CA — What is diabetes? How does it affect those who have been diagnosed with it? Although there is no cure yet, diabetes is still an urgent topic. Diabetes is a chronic disease that affects how the body turns food into usable energy. However, some misconceptions shroud its reality. With November being National Diabetes Month, the Griffin Gazette will explain this condition and how it affects those who live with it.
What is diabetes?
The body of a person without diabetes, breaks down food into sugar and releases it into the bloodstream. When the blood sugar levels go up, the pancreas releases insulin. Insulin allows for sugar to enter into cells to be used for energy.
“With diabetes, your body either doesn’t make enough insulin or can’t use it as well as it should,” according to the CDC. When not enough insulin is available, cells cannot accept insulin or the pancreas cannot produce insulin, resulting in too much sugar in the bloodstream. This leads to health risks such as heart disease, vision loss, and kidney failure.
With a low blood sugar level, a person can feel fatigued, drowsiness, and have difficulty concentrating. With a high blood sugar level, a person can feel similar symptoms, as well as increased thirst and blurred vision. Therefore, it is important for a diabetic to manage diabetes so that they can manage schoolwork, sports, or their job without any hindrances.
An estimated 26.9 million people of all ages have been diagnosed with diabetes (8.2 percent of the U.S. population). Of the people diagnosed with diabetes, 210,000 are children and adolescents younger than age 20 years, including 187,000 with type 1 diabetes.
— The National Institute of Diabetes and Digestive and Kidney Diseases
Type 1 vs. Type 2
While diabetes can be the overall term, there are two very different types, each with its treatment. However, according to Healthline, Type 1 is less common than Type 2.
Type 1 diabetes is caused by an autoimmune reaction, where the body attacks itself by mistake. In this case, the body stops itself from producing insulin.
“Approximately 5-10% of the people who have diabetes have type 1,” the CDC stated.
Type 1 is treated by the diagnosee giving insulin to themselves from an injection, a pump that automatically gives insulin, or inhaled insulin, which is when a diabetic will inhale a fast-acting powdered insulin from the mouth into the lungs, according to GoodRx Health.
Type 2 diabetes is when the body doesn’t use insulin well and is unable to keep blood sugar levels stable by itself.
“About 90-95% of people with diabetes have type 2,” the CDC said.
Another way of describing this is that the body has insulin resistance. GoodRx Health explains that a healthy diet, exercise, and weight loss are key to treating Type 2.
Continuous Glucose Monitor (CGM)
A CGM can be used to help manage and maintain a person’s diabetes. It is a device that tracks glucose levels so that the person wearing it doesn’t have to check their blood sugar manually. A tiny sensor inserted into the skin will test blood sugar levels and wirelessly transmit information to the other part of the CGM. The sensor can either send the information to a receiver that is part of an insulin pump or to a phone or other personal device. The CGM can alert the user when their blood sugar levels get too low or too high. Both children and adults can use a CGM.
“You can see your glucose level anytime at a glance,” the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) informed. “You can also review how your glucose changes over a few hours or days to see trends.”
“Most people who use CGMs have type 1 diabetes. Research is underway to learn how CGMs might help people with type 2 diabetes,” the NIDDK said.
A1C and A1C test
A1C is a term used for a blood test that diagnoses diabetes and helps to monitor treatment in a person’s A1C levels. (A1C stands for the molecule name of glycated hemoglobin: HgbA1c)
“The test results give you a picture of your average blood sugar level over the past two to three months,” The American Diabetes Association explained. The goal for most adults with diabetes is to have an A1C under 7%.
School life with diabetes
Los Alamitos High School nurse Mrs. Cassandra Palacios shared with Griffin Gazette that there are around 12 to 20 diabetic students at LAHS. Some students will come regularly to the health office to access supplies and be able to check their blood sugar levels in a safe place.
Mrs. Palacios recommended that students should learn independence when managing their diabetes and start to have less supervision.
“However, if they are not independent, then they would need to come into the health office every day,” she said.
The health office documents everything for the student, keeping a record of how often the student would come to the office, what they do to check their blood, when they give themselves insulin and at what times, and even asking the student how they feel.
“There are two types of diabetics,” Mrs. Palacios explained. “Some that are on pumps and some that use an injector or a syringe. We like to have [a] backup of everything that they like to use.” Mrs. Palacios gave examples such as a glucometer, batteries, extra insulin, glucose tabs and gel that act quickly in emergency situations, as well as other snacks and juices with sugar in them.
Mrs. Palacios said that one common misconception about diabetes is the difference between Type 1 and Type 2. Even though there may be more of one type of diabetes at school than the other, each will follow its own guidelines depending on the situation and lifestyle. They are two very different chronic diseases that just fall under the same category.
She added that another myth is that diabetics cannot eat normally like non-diabetics.
They can still eat, they can have things with sugar, they can have sweets, but they just have to go out of their way and correct it with insulin. They can, [but] they just have to pay attention to their carbohydrates and [sugar levels].
— Mrs. Palacios
She described that for athletic activities, a student would have to check their blood sugar before practice or a game and need to keep their kit of equipment with them at all times. During lunch, a student would need to take time to give themselves insulin, whether it is by themselves or in the Health Office. Even during class, if a student needed something, they could go to the health office, but then that would eat into their class time. Mrs. Palacios concluded that a diabetic student can live a normal life, but would just need to be more mindful of their condition.
Drew Massey, an LAHS senior and Type 1 diabetic, shared how diabetes affects his school life:
“In terms of academics, it’s important for me to have my blood sugar in a normal range. That way I can think normally and perform well in school. With low and high blood sugars, thinking becomes difficult, so staying on top of my blood sugar helps prevent those lows and highs.
Massey described how, with sports, being active can lower blood sugar levels, such as during games and practices. To balance this out, he has to eat something with sugar in it so that his glucose levels do not drop too much.
“…Lunch affects me because eating will always change my blood sugar. During lunch, I’ll figure out how many carbohydrates I’m eating and take the necessary amount of insulin to balance it out. However, no two days are the same, so sometimes my blood sugar will go a bit higher after lunch or dip down.”
One myth about diabetes he spoke of is that a low blood sugar level is treated with insulin.
“Taking insulin with a low blood sugar, especially if I am unconscious due to a severe lack of sugar in my blood, has the possibility to kill me,” he revealed. “Instead, I need sugar to raise my blood [glucose level].”
Another myth he mentioned is how there are some false cures for diabetes such as eating cinnamon or doing yoga.
“Currently there is no cure for T1D, only treatment through insulin and sugar,” he said.
Why it matters
Yes, diabetes is a misunderstood chronic disease. Yes, it is a real condition that impacts the lifestyles of many of all ages. Therefore, it should be known about and brought to attention. Next year when November turns up again, remember how it has been designated the month of this noteworthy topic.
People with diabetes have the full potential to live normal lives like everyone else. It just takes extra time and effort to keep up with everyone else.
— Drew Massey
Your donation will support the student journalists of Los Alamitos High School. Your contribution will allow us to purchase equipment and cover our annual website hosting costs.

Katie Arnoult is a sophomore at Los Alamitos High School and an editor for the Griffin Gazette. She was the Editor-In-Chief for the McAuliffe Birdwatch...












Cindy Maiden • Nov 22, 2022 at 6:19 pm
Thank you for this article.